When that shooting pain radiates down your leg, the first question that comes to mind is: “How long does sciatica last?” Sciatica pain typically resolves within 4–6 weeks with proper care, though some cases persist longer depending on the underlying cause. Understanding the symptoms of sciatica and which recovery strategies actually work can help you get back to normal life faster.
Let’s explore what’s causing your discomfort and when it’s time to seek specialized sciatica treatment.
What Is Sciatica?
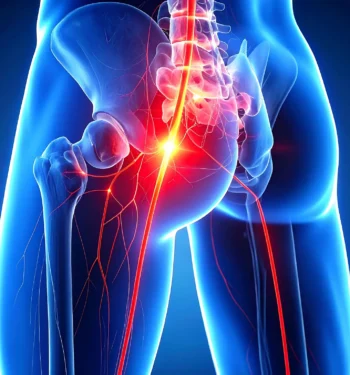
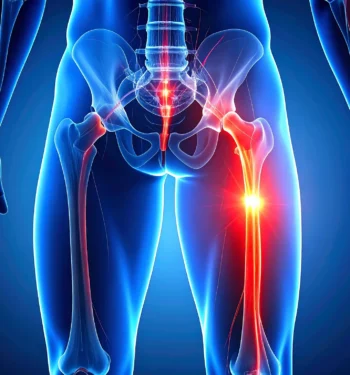
Sciatica is nerve pain that occurs when the sciatic nerve becomes compressed or irritated anywhere along its path from your lower back through your hips and down each leg. The sciatic nerve is the longest nerve in your body, which explains why sciatic nerve pain can be so intense and widespread.
You’ll typically feel the symptoms of sciatica on one side of your body — a sharp, burning sensation or electric shock radiating through your buttock and down the back of your thigh and calf, along with numbness, tingling, or muscle spasms in the affected leg.
What Causes Sciatica?
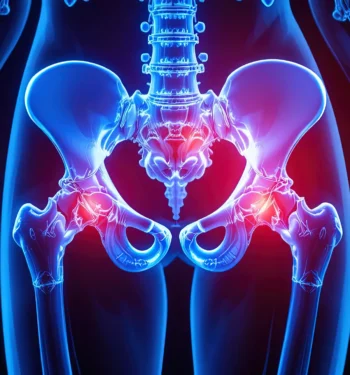
A herniated disc is the most common culprit, pressing directly on the sciatic nerve roots in your lumbar spine and triggering nerve irritation. Spinal stenosis ranks as another frequent cause, particularly in adults over 50 — this narrowing of the spinal canal puts pressure on the nerve endings that form the sciatic nerve. Other conditions include degenerative disc disease, bone spurs, or spinal cord compression.
Spinal stenosis ranks as another frequent cause, particularly in adults over 50. This narrowing of the spinal canal puts pressure on the nerve endings that form the sciatic nerve. Other conditions include degenerative disc disease, bone spurs, or spinal cord compression.
The specific cause matters because it influences both how long your symptoms will last and which treatments will be most effective.
How Long Does Sciatica Take to Fully Heal?
Most cases of acute sciatica improve significantly within 4–6 weeks. According to research published in the British Medical Journal, approximately 60% of patients with sciatica recover within 6 weeks with conservative care.
Your healing timeline depends heavily on what’s causing the nerve compression. A mild herniated disc might settle down relatively quickly as inflammation decreases. However, more significant structural problems like severe spinal stenosis or more pronounced disc herniations may take longer to resolve or might not improve without intervention.
What’s the Difference Between Acute and Chronic Sciatica?
Acute sciatica refers to symptoms present for less than 4 weeks. This initial phase often involves significant inflammation around the compressed nerve, and many acute cases resolve on their own with rest and basic care.
Chronic sciatica means symptoms have persisted beyond 12 weeks. At this stage, the underlying structural problem hasn’t typically been resolved, and the nerve may have sustained more significant irritation. Chronic sciatica often indicates you need more than time and basic home remedies to achieve lasting relief.
The transition from acute to chronic represents an important decision point. While patience makes sense in the early weeks, persistent symptoms beyond 3 months suggest the underlying cause requires professional evaluation.
For guidance on managing day-to-day sciatica pain, see our article on whether it is better to sit or lie down with sciatica.
What Influences How Long Your Sciatica Lasts?
Understanding how long does sciatica last in your specific case depends on several key factors. Not all cases of sciatica pain follow the same timeline, and knowing what drives duration can help you and your care team make better treatment decisions.
Underlying Cause
A mild nerve irritation from a small disc bulge may resolve in weeks as inflammation subsides. More significant structural problems — such as severe spinal stenosis or a large herniation — tend to take longer and may not improve without professional intervention.
Treatment Approach
Patients who begin conservative care early — combining physical therapy, anti-inflammatory medications, and activity modification — tend to experience faster pain relief than those who rely on bed rest alone. Massage therapy can also help reduce muscle spasms that contribute to prolonged nerve irritation, and is a useful complement to a structured treatment plan.
Research published in Spine Journal (PubMed) found that active exercise therapy significantly reduces duration of sciatica pain compared to passive rest, supporting the value of early physical therapy in shortening long does sciatica timelines.
Age and Overall Health
Younger, healthier patients tend to recover more quickly. Conditions such as diabetes, obesity, or pre-existing spinal stenosis can extend recovery and make symptoms of sciatica harder to alleviate symptoms through conservative means alone.
Severity of Nerve Compression
Mild nerve irritation often produces temporary sciatica pain that resolves with conservative care. Severe compression causing progressive weakness, loss of reflexes, or bowel and bladder changes typically requires surgical intervention to achieve lasting pain relief.
Can Sciatica Become a Long-Term Condition?
Yes — when left untreated or inadequately managed, sciatica can develop into chronic sciatica that persists for months or years. Chronic sciatica is defined by sciatica pain lasting beyond 12 weeks and is associated with ongoing nerve irritation, progressive muscle spasms, and reduced quality of life.
Conditions such as untreated spinal stenosis, recurring disc herniations, or persistent structural instability in the lumbar spine are the most common drivers of chronic sciatica. In these cases, conservative care alone is rarely sufficient to fully alleviate symptoms, and neurosurgical evaluation becomes important.
According to a long-term outcomes study in The Lancet (PubMed), a significant proportion of patients with chronic sciatica who did not receive surgical intervention continued to report sciatica pain at one and two years, highlighting the importance of timely specialist evaluation.
Can Sciatica During Pregnancy Become Long-Term?
Sciatica during pregnancy is often temporary, caused by the growing uterus placing pressure on the sciatic nerve. However, if symptoms of sciatica persist postpartum, an underlying structural cause such as a herniated disc may be responsible and should be evaluated.
Learn more about sciatic nerve pain during pregnancy and how to alleviate symptoms safely.
Can Sciatica Affect Both Sides?
While most cases of sciatica pain affect one side, bilateral sciatica — involving both legs — can occur and often indicates more significant nerve compression. Bilateral symptoms of sciatica typically warrant faster specialist evaluation.
See our dedicated guide on bilateral sciatica to understand when symptoms affecting both sides require urgent care.
How Can I Speed Up My Sciatica Recovery?
Gentle movement speeds recovery better than complete bed rest. Short walks and basic stretches help reduce nerve irritation and prevent muscle spasms that can worsen sciatica pain.
Physical therapy provides targeted exercises to reduce pressure on the sciatic nerve. Massage therapy can complement this by relaxing tense muscles that contribute to nerve irritation. Anti-inflammatory medications provide pain relief while your body heals. The most important factor, however, is addressing the root cause — if spinal stenosis or a herniated disc is compressing your nerve, conservative measures can alleviate symptoms but won’t fix the structural problem.
Anti-inflammatory medications can help manage pain while your body heals. Ice during the first few days can reduce acute inflammation, while heat therapy later may ease muscle tension.
The most important factor in speeding recovery is addressing the root cause. If a herniated disc or spinal stenosis is compressing your nerve, conservative measures may help, but they won’t fix the structural problem. This is where evaluation by a neurosurgeon becomes valuable.
Is It Better to Sit or Lie Down With Sciatica?
Both prolonged sitting and extended bed rest can worsen sciatica pain. Sitting increases pressure on your lumbar spine discs by up to 40% compared to standing, which can aggravate herniated disc symptoms.
When you do sit, use proper posture with lumbar support and take frequent breaks to stand and walk every 20–30 minutes. Lying down with a pillow under your knees or on your side with a pillow between your knees often feels most comfortable. These positions help maintain your spine’s natural curves and reduce pressure on the affected nerve.
When Should You See a Spine Specialist for Sciatica?
See a spine specialist immediately if you experience loss of bladder or bowel control, progressive leg weakness, or numbness — these suggest severe nerve compression requiring urgent evaluation. Schedule an appointment with a neurosurgeon if your sciatica pain hasn’t improved after 6 weeks of conservative treatment, as persistent symptoms of sciatica at this point indicate the underlying condition likely won’t resolve on its own.
Schedule an appointment with a neurosurgeon if your sciatic pain hasn’t improved after 6 weeks of conservative treatment. Persistent symptoms at this point indicate the underlying condition likely won’t resolve without professional intervention.
The difference between neurosurgeon expertise and general orthopedic care matters significantly for complex spine conditions. Neurosurgical training focuses extensively on the nervous system and intricate spinal anatomy. At Goodman Campbell, our patients gain direct access to neurosurgical specialists who treat both straightforward and complex spine conditions, backed by extensive patient outcomes data and leadership in clinical research.
How Do Neurosurgeons Treat Sciatica That Won’t Heal?
When conservative treatment fails to resolve chronic sciatica, neurosurgeons can offer several advanced options. For a herniated disc causing persistent nerve compression, a microdiscectomy removes the portion of disc material pressing on the sciatic nerve. This minimally invasive spine surgery typically provides rapid relief and requires minimal recovery time.
Spinal stenosis may require a decompression procedure to create more space around compressed nerves. In cases where spinal instability accompanies stenosis, a neurosurgeon might recommend spinal fusion to stabilize the affected vertebrae while relieving pressure. Modern minimally invasive spine surgery techniques allow neurosurgeons to address these problems through small incisions, reducing tissue damage and speeding recovery.
Can Sciatic Nerve Pain Cause Nausea?
Severe sciatica pain can trigger nausea through your body’s stress response. Medications used to treat acute pain from sciatica more commonly cause nausea as a side effect. If you’re experiencing both sciatica pain and persistent nausea, talk to your doctor about adjusting your treatment approach.
If you’re experiencing both sciatic pain and persistent nausea, talk to your doctor to rule out other conditions and adjust your pain management approach if needed.
Get Expert Neurosurgical Care for Persistent Sciatica
If sciatica pain is disrupting your life despite weeks of conservative care, the neurosurgical specialists at Goodman Campbell can provide expert evaluation and advanced treatment options for a herniated disc, spinal stenosis, and other conditions causing persistent nerve irritation.
Contact Goodman Campbell to schedule a consultation and find your most effective path to lasting relief.