Herniated Disc
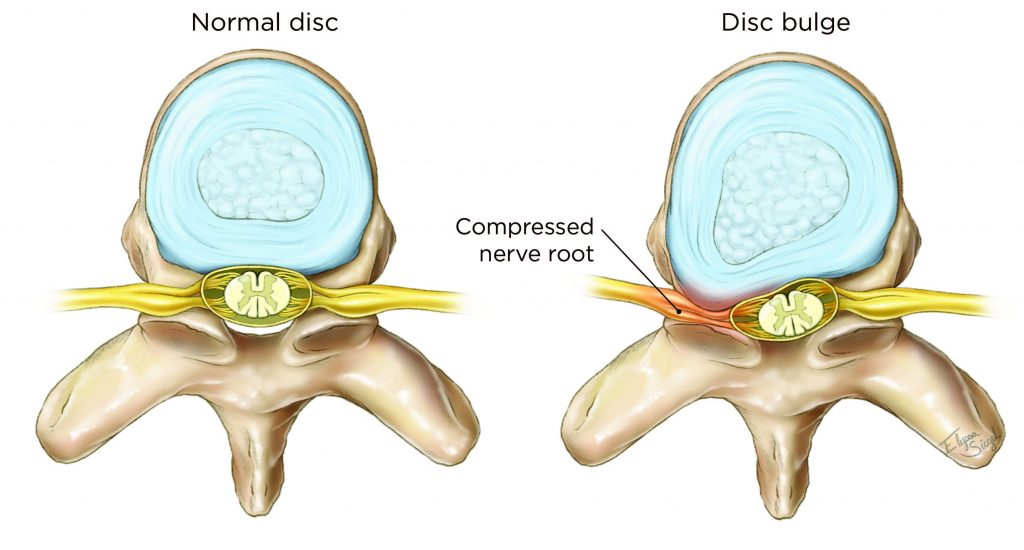
A herniated disc typically occurs when a degenerative disc breaks down, causing the disc to herniate, or protrude. This may result in pressure on or inflammation of the nearby nerves.
What’s in this section?
Signs and symptoms
Symptoms depend on the location of the herniated disc.
Lumbar disc herniations can cause the following symptoms:
- Sciatica
- Burning, tingling, numbness and pain in the leg or buttock
- Typically one sided
- Sharp pain
- Lower back pain
Cervical disc herniations can cause the following symptoms:
- Pain in the neck or between the shoulder blades
- Radiating pain down the arms
Diagnosis
Diagnosis of a herniated disc starts with a physical exam and medical history. Other procedures and tests may be needed to diagnose this condition, including x-rays , computed tomography (CT), magnetic resonance imaging (MRI) or myelogram .
Treatment options
There are a few treatment options for a herniated disc:
- Medication to reduce pain.
- Physical therapy to strengthen the area around the disc.
- Epidural steroid injections. This procedure is used to inject a steroid and a local anesthetic into the space around your spine to help decrease inflammation and swelling, typically leading to improvement in pain in your neck, arms, back and legs. It is performed in either the office or surgery center setting. This procedure typically takes just a few minutes and may be performed either with just local anesthetic or IV sedation in the surgery center, depending on patient preference. Most procedures involve a needle that is advanced to the target area using fluoroscopic (x-ray) guidance. A small amount of x-ray contrast will be injected to confirm accurate placement. Once the needle has been properly placed, a combination of a local anesthetic and/or injectable steroid will be placed into the targeted area.
- Herniated disc resection. You will be positioned face down on a padded frame/bed. By opening the skin and muscle layers, the spine is exposed. Either part of the roof (laminotomy) or the entire roof (laminectomy) is performed, depending on how much exposure is needed for the operation. When surgery is done, the retractors are removed, allowing the muscles to cover the exposed canal, and the skin is closed.
- Minimally invasive discectomy/decompression. During surgery, a small incision will be made. Your surgeon will remove bone and ligament to get access to the spinal canal. Using a microscope, the nerve will be identified, and the pressure from will be taken off by removing disc material. During this surgery, no fusion will be performed. Surgery usually takes 1 – 2 hours and typically you go home the same day.
- Disc decompression and fusion. An incision is made, depending on the location of the disc. The tissue surrounding the disc is dissected until the spine is seen. We remove the disc starting superficially, then deeper in the joint space until we work all the way through the joint and enter the spinal canal, where the bone spurs or disc herniation compresses the nerves. We remove the compressive pathology very carefully, as the nerves that are in that area are very delicate. After we get all of the pressure off of these delicate nerves, we then reconstruct the joint using an implant of cadaver bone or a cage made of synthetic materials. A metal plate and screws then are secured to the front of that part of the spine so that the bones of that segment will heal/fuse and remain stable. The wound is closed with stitches under the surface that dissolve after the skin has healed.
- Artificial disc replacement. An incision is made and the tissue planes are separated until the surgeon gets down to the spine. The disc is then removed slowly in small pieces and the pressure is pulled away from the spinal cord and/or nerve roots. An artificial disc, which can be made from many different materials depending on the manufacturer, is put into the space where the disc once was. This artificial disc has to be precisely placed so that it provides similar motion to the original disc.
Herniated Disc Treatment in Indiana FAQs
A herniated disc can significantly disrupt your life, bringing pain, discomfort, and limitations to your daily activities. At Goodman Campbell, we specialize in advanced herniated disc treatment in Indiana, offering solutions tailored to your health and lifestyle. Whether you’re exploring treatment options or seeking expert care, this FAQ will answer your top questions and help guide you toward confident decisions.
Frequently Asked Questions
A herniated disc, also known as a slipped or ruptured disc, occurs when the soft center of a spinal disc pushes through its tougher exterior.The tough outer layer of the disc can rupture, allowing the soft center to push out and irritate nearby nerve roots. This condition often affects the intervertebral discs in your cervical (neck) and lumbar (lower back) spine, impacting the vertebrae and the spinal discs, which act as shock absorbers for the spinal column. The spinal canal houses the spinal cord and nerves, and herniated discs can compress these structures, leading to a range of symptoms.
Common Symptoms and Impact:
- Pain that radiates to the arms, shoulders, or legs based on the affected area
- Numbness and tingling, often in the limbs
- Weakness, interfering with activities including walking and lifting items
Herniated disc symptoms vary depending on the location and severity of the disc herniation.
Risk factors for herniated discs include heavy lifting, repetitive activities, injury, disc degeneration (a normal part of aging), and other risk factors, especially those related to one’s occupation or genetics. Spinal stenosis can occur when the spinal canal narrows due to disc herniation or degeneration, causing nerve compression. A thorough medical history is important for accurate diagnosis.
Your quality of life may deteriorate due to limited mobility, disrupted sleep, and interference with daily activities. Herniated discs may require treatment to relieve pressure on the spinal cord and nerve roots. Seeking an expert evaluation is critical to improving spine health and ensuring you receive personalized care.
Goodman Campbell, a trusted name in Indiana, specializes in diagnosing and treating herniated discs, ensuring superior care tailored to your unique needs.
If you’re wondering, “Who is the best doctor to see for a herniated disc in Indiana?” the answer lies in choosing the most experienced professionals with specialized training in spine health.
Why Choose Goodman Campbell?
- Fellowship-Trained Neurosurgeons & Spine Specialists
- At Goodman Campbell, our team includes the best spine specialists, interventional pain management physicians, and neurosurgeons in Indiana, skilled in both surgical and nonsurgical treatments for herniated discs.
- Team-Based Approach
- Each patient’s case is reviewed collaboratively, ensuring the most effective treatment plan tailored to your condition.
- Independent Practice for Personalized Care
- Unlike many larger hospital groups, Goodman Campbell offers flexibility in choosing the best facility and treatment choices for you, always keeping patient-centered goals in mind.
Remember, a personalized treatment plan delivered by Goodman Campbell’s neurosurgeons and care team can make all the difference. Ask your doctor about Goodman Campbell’s spine specialists today.
The most frequently recommended treatment for herniated discs in Indiana isn’t a one-size-fits-all solution. Goodman Campbell takes a holistic approach, with your final treatment path depending on a variety of factors, including your symptoms, overall health, and the severity of the herniation.
Common Treatment Options Include:
- Conservative Treatments
- Physical therapy to strengthen supporting muscles
- Pain-relieving medications for temporary relief
- Activity modifications to reduce pressure on the spine
- Pain Management Solutions
- Epidural Steroid Injections to reduce inflammation and relieve paid
- Surgical Treatments
- Micro Lumbar Discectomy: Patients seeking information about micro lumbar discectomy in Indiana learn that the minimally invasive procedure is done to remove the herniated portion of the disc.
- Minimally Invasive Spine Surgery: Designed to reduce tissue disruption and shorten recovery time, minimally invasive spine surgery can offer lasting relief with smaller incisions, less postoperative pain, and a quicker return to normal activities. This approach is often ideal for patients seeking effective treatment with fewer risks and a more comfortable healing process.
Imaging is important for accurate diagnosis. Goodman Campbell carefully reviews each patient’s imaging, such as high-resolution MRI, 3D CT-guided navigation and X-rays, to enhance diagnostic precision and surgical accuracy.
When exploring any procedure, patients should consider the surgeons’ experience level and track record of successful recovery outcomes. Don’t be shy about asking for quantitative data about patient outcomes and satisfaction.
At Goodman Campbell, we stay on the cutting edge of advanced spine care with multidisciplinary team reviews to ensure every patient has access to the best herniated disc treatment options.
Request an appointment or ask your doctor about the state-of-the-art spine care available at Goodman Campbell today.
One of the most common questions patients ask is, “How much does it cost to fix a herniated disc?” While the cost of herniated disc treatment in Indiana depends on several variables, Goodman Campbell provides transparent information and financial counseling for your peace of mind. Specific cost variables can include:
- Type of treatment (conservative vs. surgical)
- Severity of the herniation
- Surgical approach (minimally invasive procedures can be more cost-effective)
Insurance Coverage
Goodman Campbell works with most private insurance providers to ensure affordability while offering premium care. We also help patients understand their insurance plans and financing options.
How Goodman Campbell Can Save You Money
If you are a good candidate for minimally invasive outpatient spine surgery, choosing such a procedure can not only reduce overall expenses, but it can also reduce recovery times, letting you get back to your life and job faster.
Ask your doctor about Goodman Campbell and discuss your insurance coverage to explore cost-effective treatment plans.
With decades of experience, Goodman Campbell has become the go-to choice for Indiana spine specialists. Here’s why:
Outstanding Expertise
- From simple herniated discs to complex spine conditions, we excel in providing advanced spine care.
Comprehensive Care
- Whether you are visiting one of our conveniently located outpatient clinics or seeing one of our on-call physicians inside a hospital, Goodman Campbell delivers exceptional patient outcomes for the simplest to the most complex neurosurgical cases.
Commitment to Patient-Centered Results
- We regularly measure and optimize patient outcomes, ensuring satisfaction through high-quality care.
When you choose Goodman Campbell, you’re not just selecting a treatment provider. You’re partnering with a team dedicated to helping you reclaim your mobility and enrich your quality of life.
Talk to your doctor about Goodman Campbell’s herniated disc treatment in Indiana and take the first step toward restoring your active lifestyle.
TAKE CONTROL OF YOUR SPINE HEALTH TODAY
A herniated disc doesn’t just affect your physical health; it impacts every aspect of your life. With Goodman Campbell’s expert care, you can regain control, find relief, and live a comfortable, active life. Whether you’re seeking conservative care or surgical solutions, our advanced techniques and patient-focused approach ensure you’re in the best hands.
Contact Goodman Campbell today to discuss your options and explore personalized paths to recovery.
Conditions
Request an appointment online and we will guide you through the next steps
Get to know the physicians of Goodman Campbell
Goodman Campbell
Patient Stories
Request an appointment online and we will guide you through the next steps.
