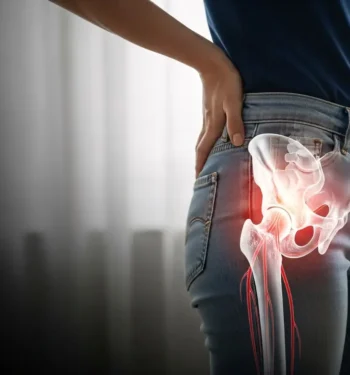
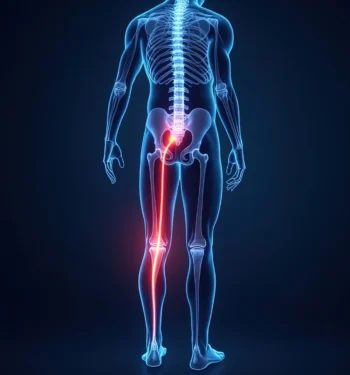
When unexpected pain strikes in your lower back, hips, or legs, understanding whether you’re dealing with piriformis syndrome vs sciatica is a smart first step toward effective healing. Both conditions can cause significant discomfort, but they differ in their origin and the piriformis syndrome treatment or sciatica care required.
Request an appointment or ask your doctor about Goodman Campbell to get an expert diagnosis and compassionate treatment plan personalized just for you.
What Is Piriformis Syndrome?
Piriformis syndrome occurs when the piriformis muscle — located deep in the buttock — spasms, tightens, or becomes inflamed, and the piriformis muscle compresses the nearby sciatic nerve. This type of nerve compression typically causes pain piriformis syndrome that begins in the buttock and may radiate down the back of the leg, often worsening with sitting, climbing stairs, or prolonged activity.
Common symptoms piriformis syndrome include localized tenderness, tingling, and discomfort that starts in the hip rather than the lower back. Because this condition is muscular rather than spinal, piriformis syndrome treatment usually focuses on stretching, physical therapy, posture correction, and anti-inflammatory strategies to relieve pressure on the nerve.
What Is Sciatica?
In the discussion of piriformis syndrome vs sciatica, sciatica is not a condition itself but a set of symptoms caused by irritation or nerve compression of the sciatic nerve, most often originating in the lower spine. Issues such as a herniated disc, bone spur, or spinal stenosis can place pressure on the nerve roots, leading to pain that typically starts in the lower back and travels through the buttock and down the leg. Unlike piriformis-related pain, true sciatica is usually linked to spinal pathology and may be accompanied by numbness, weakness, or changes in reflexes along the nerve pathway.
Anatomy of the Sciatic Nerve and Piriformis Muscle
The piriformis muscle is a pear-shaped muscle that runs from the lower spine through the buttock to the top of the thigh bone. Its close relationship with the sciatic nerve means even minor dysfunction — such as when the piriformis muscle compresses the nerve — can cause significant pain piriformis syndrome that presents like classic sciatica.
Why Is Distinguishing Between Piriformis Syndrome and Sciatica Important?
Knowing whether you have piriformis syndrome or sciatica ensures you receive the right treatment. Their pain patterns often overlap, but piriformis syndrome treatment differs significantly from treatment for spinal-origin sciatica. An early, precise diagnosis reduces recovery time and prevents unnecessary suffering. Ask your doctor about Goodman Campbell for expert guidance.
What Is the Difference Between Sciatica and Piriformis Syndrome?
While piriformis syndrome vs sciatica can look similar on the surface, four key areas help distinguish them:
- Where pain starts: In piriformis syndrome, pain piriformis syndrome originates deep in the buttock at the site where the piriformis muscle compresses the sciatic nerve. In true sciatica, pain originates in the lower back or lumbar spine where a structural problem compresses the nerve roots.
- Primary cause of nerve irritation: Piriformis syndrome occurs due to a muscular cause — the piriformis muscle tightening or spasming around the sciatic nerve (nerve compression from outside the spine). Sciatica is caused by spinal pathology such as a herniated disc, bone spur, or stenosis compressing the nerve roots inside the spine.
- Activities that worsen symptoms: Symptoms piriformis syndrome are typically aggravated by activities involving hip rotation — sitting for long periods, climbing stairs, or getting out of a car. Sciatica pain tends to worsen with spinal movements such as bending forward, prolonged standing, or sneezing.
- Whether pain extends below the knee: Sciatica frequently radiates all the way down the back of the calf and into the foot, following the sciatic nerve pathway. Pain piriformis syndrome usually stays closer to the buttock and upper thigh — in most cases, it does not extend below the knee.
For guidance on which specialist to see for these conditions, read our article on what kind of doctor treats sciatica.
How Do You Know if You Have Sciatica or Piriformis Pain?
Differentiating between piriformis syndrome and sciatica can be challenging, as both conditions involve nerve compression that causes leg pain. Understanding the pain pattern and recognizing what triggers your discomfort are the first steps in a proper diagnosis. If you’re unsure about your symptoms piriformis syndrome vs. sciatica, request an appointment or ask your doctor about Goodman Campbell for an expert evaluation.
Typical Symptoms of Sciatica
Sciatica typically results from nerve compression caused by issues in the lower back such as a herniated disc or spinal stenosis. Common symptoms include sharp, shooting pain radiating from the lower back through the buttock and down the back of one leg, accompanied by numbness, tingling, or weakness. The pain usually worsens with prolonged sitting, standing, or bending.
Piriformis Syndrome Pain Pattern
Pain piriformis syndrome generally starts deep in the buttock and may radiate along the path of the sciatic nerve, but typically does not originate in the lower back. The discomfort worsens after sitting for extended periods or with hip-rotation activities. Localized tenderness over the piriformis muscle in the buttock region is a notable differentiating sign of piriformis syndrome.
Differences in Pain Location, Triggers, and Associated Symptoms
While both conditions cause leg pain, sciatica starts in the lower back and moves downward, whereas piriformis syndrome occurs in the buttock. Sciatica follows a predictable path along the back of the thigh and calf, sometimes reaching the foot. Pain piriformis syndrome is usually limited to the buttock and upper thigh, rarely extending below the knee. Activities that stretch or contract the piriformis muscle provoke symptoms piriformis syndrome, while classic sciatica is aggravated by spinal movements.
When to Use a Piriformis Syndrome vs. Sciatica Test
Certain physical tests can help distinguish between piriformis syndrome vs sciatica, but self-diagnosis carries risks due to overlapping symptoms piriformis syndrome. The most reliable path is partnering with a specialist who can tailor questions and tests to your unique situation. Ask your doctor about Goodman Campbell for a clear diagnosis.
Can You Have Piriformis Syndrome and Sciatica at the Same Time?
Yes — it is possible to experience both piriformis syndrome and sciatica simultaneously. This overlap occurs because piriformis syndrome occurs with nerve compression of the very nerve that produces sciatica symptoms. When the piriformis muscle spasms, the piriformis muscle compresses the sciatic nerve directly — either causing or worsening sciatica.
How Piriformis Syndrome Can Cause or Mimic Sciatica
Piriformis syndrome often presents with symptoms piriformis syndrome — pain, tingling, or numbness radiating from the buttock down the leg — that closely resemble classic sciatica. However, while sciatica traditionally stems from nerve compression in the lower back, piriformis syndrome occurs in the buttock. Without a thorough medical evaluation, many patients struggle to distinguish the two.
Explanation Of Overlapping Conditions
When patients experience both conditions simultaneously, the tight or injured piriformis muscle directly contributes to sciatic nerve compression, amplifying the overall pain piriformis syndrome and sometimes leading to severe symptoms that affect daily mobility.
Risk Factors for Simultaneous Presentation
Risk factors include repetitive lower body movements, prolonged sitting, trauma to the buttock or hip, and muscular imbalances — all of which can drive piriformis syndrome to worsen existing sciatica.
For treatment options that address both conditions, see our article on lumbago with sciatica treatment options.
Guidance on When to Ask Your Doctor About Goodman Campbell
If you ever experience persistent pain in your lower back or buttocks that radiates down your leg, or feel numbness, tingling, or weakness, it’s important not to ignore these symptoms. Especially if both piriformis syndrome and sciatica symptoms appear together, consult a medical professional for an accurate diagnosis and a targeted treatment plan. It’s important to remember that every patient’s journey is unique. For comprehensive care and lasting relief, ask your doctor about Goodman Campbell, where compassionate experts are dedicated to helping you find hope, healing, and a return to the activities you love.
What Is The FAIR Test For Piriformis Syndrome?
The FAIR test — which stands for Flexion, Adduction, and Internal Rotation — is a specialized physical exam maneuver that helps healthcare professionals assess for piriformis syndrome. By positioning the hip in a certain way and applying gentle pressure, the FAIR test can help reproduce symptoms and aid in distinguishing piriformis syndrome from other causes of buttock or leg pain. However, while the test is helpful, it is only one piece of a thorough evaluation, and interpretation is best left to a qualified medical provider.
For a helpful educational overview of musculoskeletal and nerve-related assessment, see this resource from BBC Bitesize, which covers how nerve-related conditions of the musculoskeletal system are assessed — relevant context for understanding tests like the FAIR assessment.
Step-by-Step Explanation of the FAIR (Flexion, Adduction, Internal Rotation) Test
During the FAIR test, the patient typically lies on their unaffected side with the hip and knee flexed. The examiner gently moves the affected leg into flexion, adduction, and internal rotation. If this position causes pain piriformis syndrome in the buttock or reproduces typical symptoms piriformis syndrome, it suggests irritation or nerve compression of the piriformis muscle. This test should only be performed by a healthcare professional.
Other at-Home or Clinical Tests for Distinguishing Piriformis Syndrome
While the FAIR test is widely used, gentle stretches that place the hip in similar positions may reproduce symptoms piriformis syndrome at home — though these are not as reliable as in-clinic diagnostic tests and should be done carefully. A full diagnosis of piriformis syndrome vs sciatica requires a comprehensive evaluation.
Limitations of Self-Testing and When to Seek Expert Evaluation
An accurate diagnosis for piriformis syndrome or sciatica involves physical examination, detailed history, and sometimes imaging or advanced diagnostics. If your symptoms piriformis syndrome are persistent, worsening, or interfering with daily life, seek professional medical advice. Ask your doctor about Goodman Campbell.
Importance of Professional Diagnosis — Ask Your Doctor About Goodman Campbell
Goodman Campbell’s experienced care team uses the latest diagnostic tests to assess your pain piriformis syndrome and design a tailored piriformis syndrome treatment plan. Request an appointment to fast-track your path to relief.
How Do You Release the Sciatic Nerve From the Piriformis?
Releasing the sciatic nerve from piriformis muscle compresses is an essential step toward pain relief. This can often be addressed with targeted piriformis syndrome treatment exercises, gentle stretching, and therapeutic strategies that promote healing while reducing nerve compression.
For the most effective approaches to piriformis syndrome treatment and lasting relief, explore our article on the most successful treatment for sciatica.
Effective Stretches and Exercises for Piriformis Syndrome
Relieving sciatic nerve pressure can start by adopting simple, daily stretching routines — always with permission from your healthcare provider. Gentle movements like the supine piriformis stretch, figure-four stretch, or walking hip stretches can effectively target and relax a tight piriformis muscle. These piriformis syndrome exercises work by enhancing flexibility and increasing blood flow to the affected area, and can reduce nerve compression and bring tangible pain relief. Remember to move slowly and be patient. Consistency is key to long-term comfort and healing.
Tips for Quick Relief: Ice, Heat, and Position Changes
If you want to know how to heal piriformis syndrome quickly, you may need to temper your expectations. Following an expert-guided exercise and stretching program is critical to healing and will take time. To alleviate symptoms while you heal, integrating immediate relief measures into your day-to-day life has the potential to be a transformative choice. Such measures include applying ice packs to help reduce inflammation after activity and heat therapy — such as warm baths or heating pads — to relax the piriformis muscle and ease tension on the sciatic nerve. Adjusting your posture, avoiding prolonged sitting, and gently changing positions throughout the day can further prevent pinching of the nerve and reduce discomfort.
Role of Physical Therapy and Guided Rehabilitation
Often, the most effective pathway to sustained healing comes from guided physical therapy. Skilled therapists can provide individualized stretches, strength-building routines, and manual techniques to target the root cause of your pain. With expert input, you’ll learn how to perform exercises correctly, enhance your body mechanics, and lower the likelihood of recurrence. If you are searching for inspiration and progress in your healing journey, physical therapy often provides both immediate and long-term benefits.
Treatment Options and When to Consult a Specialist at Goodman Campbell
While home-based exercises and lifestyle adaptations are powerful first steps, some individuals may require advanced care. Persistent or severe pain, numbness, or weakness in the leg may signal the need for a comprehensive evaluation by a specialist. Goodman Campbell offers a range of solutions, including diagnostic testing, image-guided injections, and, in rare cases, surgical intervention when conservative measures have not provided relief. Listen to your body and remember: for expert assessment and compassionate support, ask your doctor about Goodman Campbell today to take the next step towards renewed healing and health.
Prevention, Recovery, and When to Ask Your Doctor About Goodman Campbell
Prevention is key to ensuring the pain and discomfort of piriformis syndrome or sciatica do not return. Practicing regular piriformis syndrome exercises that stretch and strengthen the piriformis muscle can help you maintain flexibility and resilience in this region. Incorporating a short stretching routine — especially prior to extended periods of sitting, exercise, or strenuous activity — can make a significant difference in keeping symptoms at bay. Good posture, proper ergonomics at work or while driving, and staying active with low-impact exercise such as walking or swimming are essential steps for ongoing prevention.
What Are Simple Tips to Prevent Recurrence of Piriformis Syndrome or Sciatica?
To minimize your risk of another episode, it’s helpful to listen to your body and recognize early signs of tension or discomfort. Use a supportive chair, avoid crossing your legs for long periods, and take standing or stretching breaks every 30–60 minutes during sedentary work. Additionally, practicing safe lifting techniques and maintaining a healthy weight can reduce unnecessary stress on your hips and lower back. Preventing falls or injuries through regular balance and core exercises also supports ongoing musculoskeletal health.
What Long-Term Management Strategies Keep Pain Away?
Long-term management means blending lifestyle adjustments with ongoing care. Many patients benefit from continuing physical therapy or adopting at-home guided exercise routines. Alternative therapies such as massage or yoga can relieve tension. Mindfulness, stress reduction, and staying hydrated all play roles in supporting nerve and muscle health. For those who have experienced recurrent piriformis or sciatic pain, establishing a relationship with a spine specialist who can monitor your progress is a valuable strategy, especially if new symptoms arise.
When Should You Consult a Medical Professional?
If you notice that your pain returns frequently, is not improving with home care, or includes new neurological symptoms such as numbness, significant weakness, or loss of bowel or bladder control, it’s time to seek expert evaluation. Early intervention can prevent complications and give you assurance that the most effective and least invasive treatments are being considered. Do not hesitate to reach out when home measures fall short; your well-being is worth the extra attention.
How Can Goodman Campbell Help With Diagnosis, Treatment, and Ongoing Care?
At Goodman Campbell, the focus remains on patient-centered, compassionate care throughout your journey, from accurate assessment and diagnosis to tailored treatment plans and supportive follow-up. Our multidisciplinary team draws from deep experience in the management of piriformis syndrome, sciatica, and other nerve and muscle issues, ensuring that you benefit from the latest advances and evidence-based techniques. Goodman Campbell’s resources empower you and your family to make informed decisions and foster lasting recovery.
Your comfort and quality of life deserve the best care — wherever you are along your path to healing. Many Goodman Campbell patients have regained their freedom from pain and reclaimed more active lives thanks to the expert support provided by our comprehensive spine care team. If you or your loved one is ready to move forward, ask your doctor about Goodman Campbell.